Content:
What is heel pad syndrome?
Symptoms
Causes
Pain relief and treatment of heel pad syndrome
How to prevent heel pad syndrome in the future?
When to see a doctor about your heel pad pain
Heal that heel pain
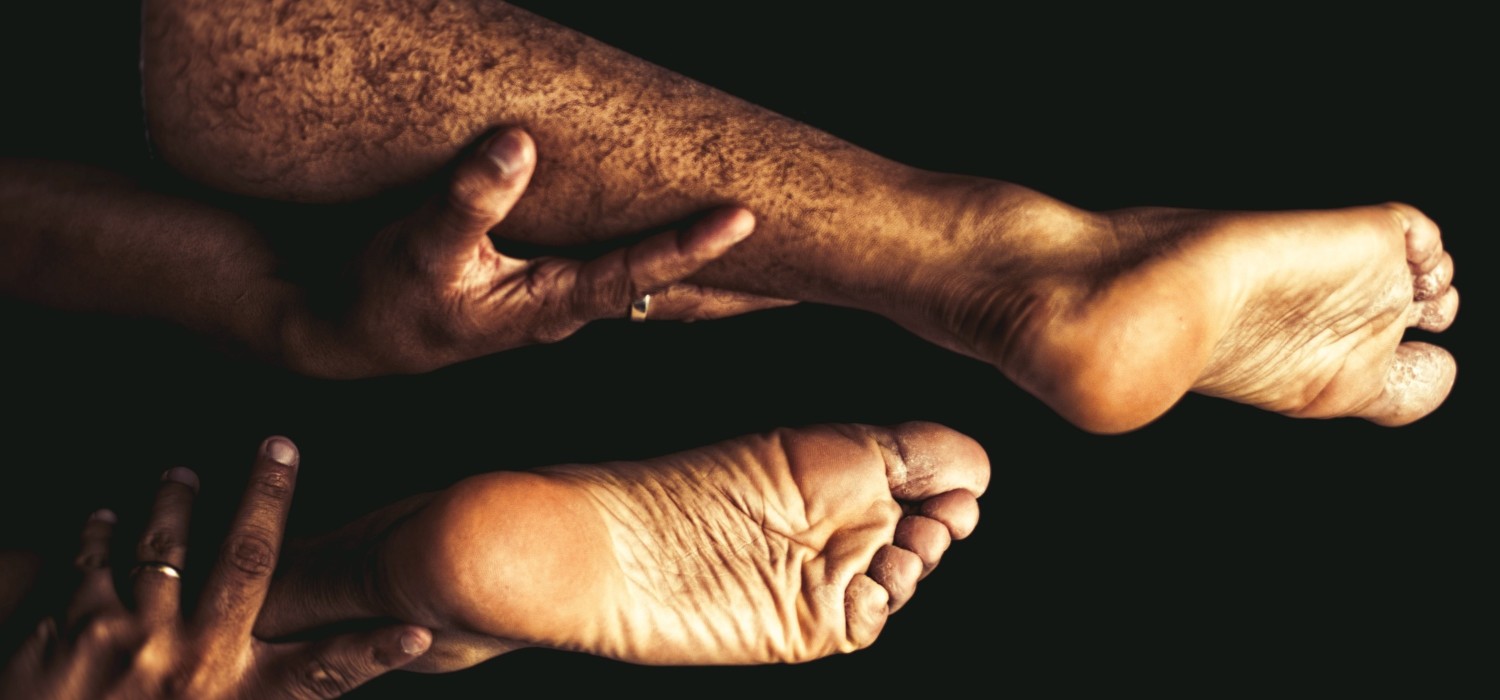
There’s a deep pain in the middle of your heel. It feels like a bruise, but you can’t see anything wrong on the surface. Yet, you find it difficult to run or even stand for long periods of time. Walking barefoot, especially on hard surfaces, is very painful.1
If any of the above symptoms sound familiar, you could be suffering from heel pad syndrome. Luckily, this is a treatable condition that can improve with exercise. But, your heel pain could also be due to other causes. How can you tell what’s causing your pain? And what can you do to treat your heel pad syndrome?
In this informative guide, we help you understand the symptoms, causes, and treatment of heel pad syndrome. We also explore how it is different from other causes of heel pain. Last but not least, you’ll learn some rehab exercises that can make your symptoms better.
Looking for a solution to heel pad syndrome? Try the Injurymap exercise app now.
What is heel pad syndrome?
Heel pads are shock-absorbing cushions in your heels. They are made of adipose tissue (fat) and tough, but flexible muscle fibers. When you stand, walk, jump, or run, your heel pads absorb the shock of the impact. They distribute your body weight and protect the bones and joints of the foot.1
Other pain relief options
Rest, ice, and pain medications: If you have symptoms of heel pad syndrome, consider taking a break from intense athletic training, such as long-distance running. Icing the heel can also relieve pain. Short-term use of pain medications, such as ibuprofen or acetaminophen, may help.7
Taping: Temporary athletic taping of the heel fat pad can provide more cushioning under the heel and reduce pain.7
Footwear modifications: Custom-molded shoes, heel cups, and cushioned socks with extra padding can support the feet and reduce the impact on the heels.8
Recovery time
Fortunately, most people recover from heel pad syndrome with conservative treatments, including exercise. Like most conditions that result from wear and tear or overuse, rest can help your feet rebuild and repair the fat pad in the heel. You can speed up your recovery by performing stretching and strengthening exercises. Low-impact weight-bearing exercises are advisable while you heal.
How is heel pad syndrome diagnosed?
Doctors make a diagnosis of heel pad syndrome based on the symptoms you describe and your physical examination. Your physician may order an X-ray or ultrasound study of your foot to diagnose fat pad atrophy or rule out other causes of heel pain.1
Doctors can measure the thickness of your heel pad on imaging studies. Normal heel pads are 1-2 cm thick. A fat pad that measures less than 1 cm in thickness is considered atrophied.8 To assess elasticity, your doctor may compare the heel pad thickness when you’re bearing weight to when you’re not.1
Complications
Untreated heel pain can be disabling, making it difficult for you to walk, play sports, and be productive at work. Heel pain can also change the way you walk, making you susceptible to falls and injuries.9
How to prevent heel pad syndrome in the future?
You can do several things to reduce your risk of developing heel fat pad atrophy:10
- Exercise regularly and maintain a healthy body weight (excess body weight is a known risk factor for heel pad syndrome).
- Avoid activities that place excessive pressure on the heels, such as walking barefoot on hard surfaces or running long distances on uneven surfaces.
- Wear comfortable, well-cushioned footwear that absorbs shock and supports your heels.
- Use insoles or shoe padding to distribute your body weight equally and minimize the impact of walking or running.
- Build strength and flexibility in your feet with regular exercise.
When to see a doctor about your heel pad pain
Most people can manage heel pain due to fat pad atrophy with home remedies and exercise.
See a doctor if:11
- You have severe pain.
- You have swelling or redness in your heel.
- You are unable to walk due to heel pain.
- Your pain does not improve after a few days of conservative home treatments.
Heal that heel pain
The symptoms of heel pad syndrome can be severe and unbearable for both athletes and non-athletes. The heel pain can keep you from running or leading an active lifestyle. Fortunately, you can treat your pain from heel pad syndrome at home with stretching and strengthening exercises.
The Injurymap app shows you several exercises to help you recover from heel pad syndrome. These exercises will relieve your pain. They will also help to build strength and flexibility and prevent the problem from recurring. Best of all, you don’t need to buy any expensive gear or cough up for a pricy gym membership. You can perform all the exercises in the convenience of your home with minimal equipment. The app shows you the correct technique to do each exercise.
If you have heel pain due to fat pad atrophy, start by doing some gentle stretches. Then, gradually scale up your workout to include strengthening exercises. Try the Injurymap app today. You’ll find it is a convenient and cost-effective way to stay in shape and speed up recovery from heel pad syndrome.
Start your 14-day free trial of the Injurymap app today!
References: